Dive Brief:
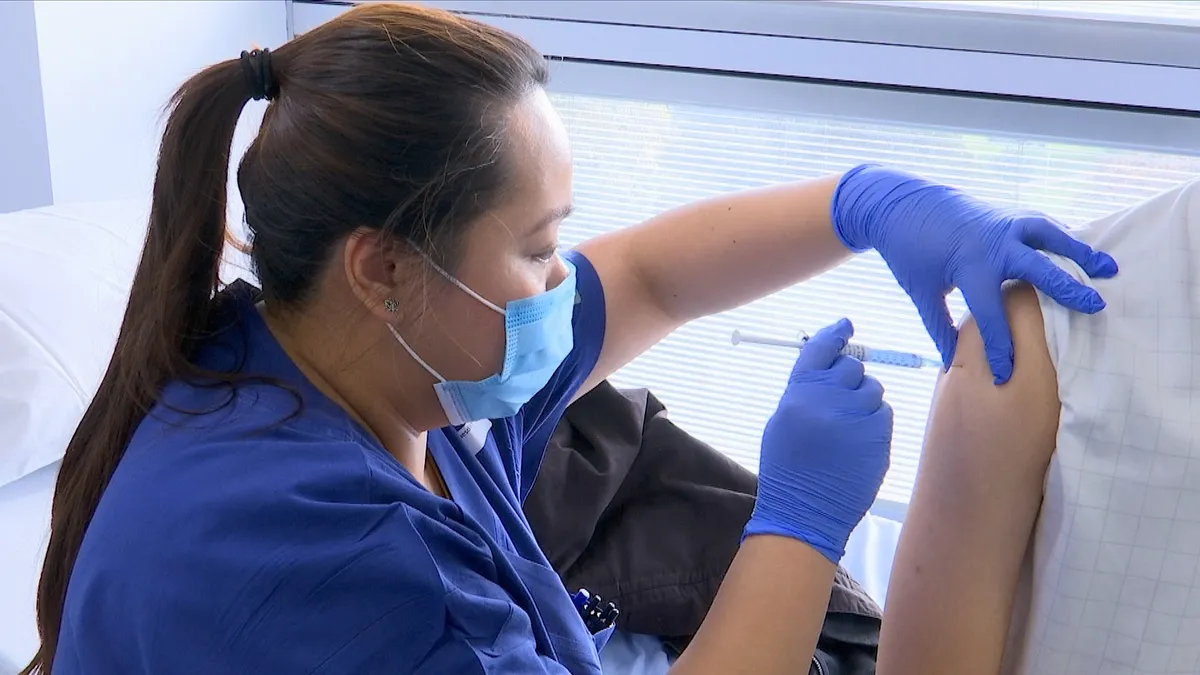
- U.S. hospitals are finalizing their plans to distribute the first doses of a coronavirus vaccine, once authorized, to their front-line staff as they face facilities at full capacity and workers burned out or falling sick themselves.
- Two Utah health systems on Thursday offered a glimpse into their processes, which will target doctors and nurses who have regularly treated COVID-19 patients, such as in the ICU or ER, as well as environmental service workers like housekeepers and other staff who handle waste.
- Neither Intermountain Healthcare nor the University of Utah Health intend to mandate staff receive the vaccine, officials said during a press conference. That could change down the road, however, when a shot receives full FDA approval.
Dive Insight:
The coronavirus vaccination timeline has become clearer in recent days and weeks as Pfizer/BioNTech and Moderna announced they have applied for FDA emergency use authorization for their shots. That's as the U.S. on Wednesday reported the highest level of COVID-19 hospitalizations since the pandemic began.
Hospitals have been preparing for vaccine distribution for months, establishing task forces and beginning the process of figuring out who will administer the doses and who will be the first to receive them. "We're really targeting those healthcare personnel that have been on the front lines taking care of our COVID patients since March," said Tamara Sheffield, Intermountain's medical director of community health and prevention.
A Centers for Disease Control and Prevention advisory panel this week overwhelming voted to prioritize healthcare workers among the first tranche in the U.S. to receive the vaccine, along with long-term care facility staff and residents.
A separate FDA panel will consider Pfizer's emergency use authorization application during a meeting Dec. 10, so the first dose could be ready theoretically to go into the arms of workers within days after that.
That vaccine has stringent storage and handling requirements, including the need for ultra-cold freezers, which Intermountain and U of U Health said they already have on hand.
"It also requires special handling, which our pharmacists, our nursing staff, all are being trained to handle," said Janemarie Mayer, epidemiologist at U of U Health. "So as soon as we receive it, and the EUA is complete, we can administer it as quickly as possible."
The health systems will receive their supplies direct from the drugmaker. Intermountain anticipates receiving about 1,000 doses for each of four designated hospitals, for example.
Those managing the vaccination plan are working with clinical leads to ensure the vaccine is staggered among care teams. They anticipate some mild side effects and don't want too many members of one team to get the dose at the same time.
Other measures may include scheduling shots before a staffer's weekend to reduce the chance of them needing to take time off to deal with symptoms.
"It's sort of been all hands on deck," Sheffield said. "And we've learned during the COVID pandemic that you have to be very flexible — things change fast. We're not quite sure when we're going to get the vaccine, but we're going to be prepared and ready for that."
Security is another concern. Intermountain and U of U Health are storing their vaccine doses in pharmacy areas, which are centrally located and locked.
That extends to cybersecurity as well. IBM on Thursday said it had uncovered a global phishing scheme targeting companies and organizations involved in the COVID-19 vaccine cold supply chain. Based on that information, the Cybersecurity and Infrastructure Security Agency issued an alert encouraging organizations involved in vaccine storage and transport to be vigilant.