Dive Brief:
- GoodRx is adding insurance coverage information to its drug cost estimation platform for providers, in what the California-based digital health company says is a key differentiator for the fast-growing tool.
- The addition of real-time benefits check to Provider Mode makes GoodRx the only platform for clinicians to compare insurance prices, cash prices and manufacturer savings programs in one place, the company said.
- Since the launch of Provider Mode in October, over 550,000 healthcare providers have used the platform, and tens of thousands of additional users are being added each month, according to Akeel Williams, general manager of GoodRx Provider Mode.
Dive Insight:
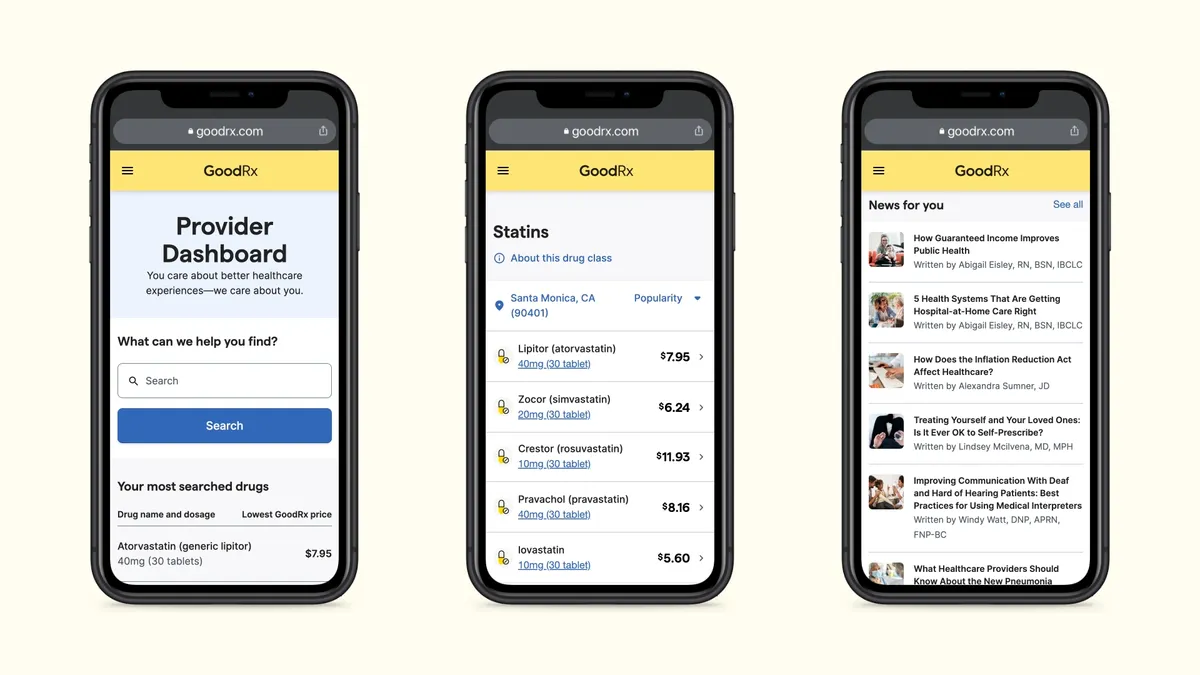
Provider Mode allows clinicians to compare cost options between different drugs during patient visits, including between different methods of payment and drug alternatives in the same class, with the goal of helping providers make more informed prescribing decisions.
Providers can also use the platform to offer GoodRx coupons and other discounts from pharmaceutical companies before patients leave the doctor's office.
But real-time benefits check is the platform’s “biggest, most transformative feature to date,” Williams said.
When providers search for a drug on GoodRx’s platform and verify their identity using their national provider identifier, they’re prompted to enter the patient’s name, date of birth, gender and zip code. GoodRx has partnered with specialty pharmacy workflow company AssistRx on the benefits check, which then pings its network of insurers and pharmacy benefit managers to find that patient’s coverage information and sends it back to the platform.
The provider can then see how much that patient will pay for that drug under their insurance, and compare it to other options.
GoodRx’s goal is to create a comprehensive view across different payment options to remove guesswork around a medication’s cost, increase adherence for patients and relieve administrative burden for doctors, Williams said.
Real-time benefits check is able to surface a patient’s insurance information about 80% of the time, as certain plans don’t participate in the AssistRx network or might experience data blackouts, Williams said.
When GoodRx is able to generate the information, it is almost always accurate, according to Williams.
“As long as we have those inputs, and they're inputted correctly, you're gonna get an accurate view, right,” Williams said. “There's always a caveat that sometimes a coupon that someone may see on a website — by the time they go to a pharmacy, because you're dealing with billions of data points, there may be some inaccuracies there.”
Currently, real-time benefits check is only available for brand and specialty drugs, though GoodRx is working to expand to generics, Williams said.
The company is also exploring additional capabilities for Provider Mode, including weaving in artificial intelligence and machine learning, though the Provider Mode GM said it’s too early to speak to specific use cases for the technology.
Provider Mode is free to providers. But by making the platform more attractive to clinician users, GoodRx is also increasing its revenue opportunities.
The platform makes money by contracting with pharmaceutical companies that want to integrate application programming interfaces and signup modules into the platform, Williams said.
The platform is also a source of revenue by serving as another referral point for GoodRx coupons.
GoodRx is paid through contracts with PBMs, either with a paid percentage of fees that PBMs charge to the pharmacy or a fixed amount for every prescription that’s filled from its discounted pricing. GoodRx is generally paid more if its coupons generate a higher volume of prescriptions over a payment period.
GoodRx has sought out new avenues to connect patients to its coupons, including through deals with PBMs.
In July, GoodRx partnered with CVS Caremark, the largest PBM in the U.S., to automatically apply GoodRx coupons for CVS commercially insured customers filling generic prescriptions at eligible pharmacies.
GoodRx has experienced mixed financial results over the past year. The company posted a profit of $58.8 million in second-quarter results announced in June, after losses ranging from $1 million to $42 million in the previous four quarters.