Dive Brief:
- Uber Health users covered by eligible Medicare Advantage plans will soon be able to use their benefit cards to pay for non-emergency medical rides and food and item delivery through the ride-hailing company’s new partnership with Optum.
- The goal of the partnership with Optum — UnitedHealth’s health services division — is to make supplemental benefits easier for beneficiaries to access, Uber said in a Sunday release.
- Members of select MA plans using the Optum-backed cards will be eligible in 2024. Uber expects to expand over time to include users covered in Medicaid and commercial health plans.
Dive Insight:
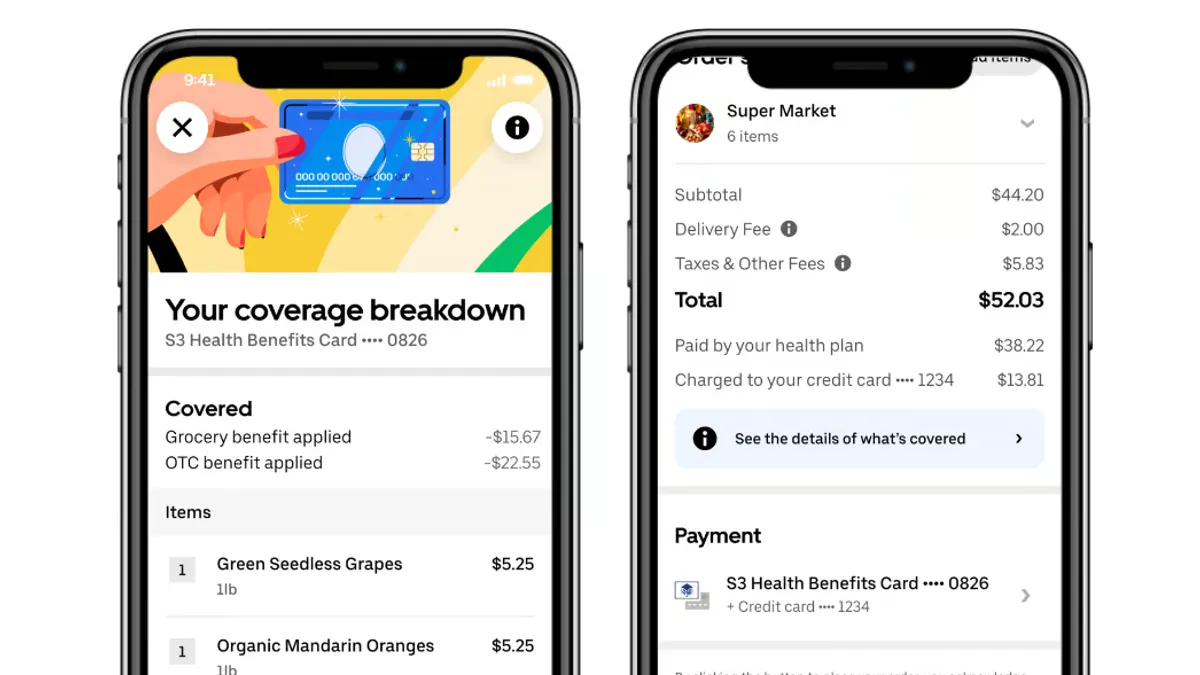
The announcement marks the first time Uber customers will be able to use health benefits cards, including health spending account (HSA) and flexible spending (FSA) cards, to know what items or services are eligible for coverage — and use those cards to pay — directly on Uber’s platform, an Uber spokesperson said.
Uber was “predominantly care coordinator and provider facing,” said Caitlin Donovan, global head of Uber Health, during a Sunday panel at the HLTH conference in Las Vegas. “Now that we have our integration with Optum Financial Services and flex cards, that is patient facing, I do think we become a patient entry point. But that’s new for us.”
An Uber spokesperson declined to share how many plans or which health insurers would participate in 2024, or the projected timeline for expansion.
The company says its goal is to make it simpler for users to find covered items in Uber’s app. But the partnership should also nudge new consumers to Uber’s health platform, which the rideshare giant first launched in 2018.
Since then, Uber has added over-the-counter item, grocery and prescription delivery as it competes against existing non-emergency transportation providers like Veyo and fellow rideshare giant Lyft, which also operates a health-specific platform.
Optum operates a health payments platform, called Optum Financial S3 Healthcare Benefits Card, that enables benefits cards. Partnering with Optum will allow Uber to configure what’s covered, including delivery and service fees, to the specifics of a particular plan, according to the spokesperson.
Optum is also a good partner for Uber due to “the breadth of Optum Financial Service’s coverage,” the spokesperson said. As of 2017, Optum managed more than three million HSAs.
Uber declined to share financial terms of the deal.
In the increasingly popular MA program, the government contracts with private plans to cover seniors’ care. Plans can offer more flexible benefits than in traditional Medicare plans, like dental coverage or subsidized gym memberships.
There have been a number of recent partnerships between MA plans and supplemental benefits providers. Payers see the services as a way to differentiate their MA plans in a highly competitive market, while it’s a strategy to expand reach for service providers.
Grocery technology company Instacart — a competitor of Uber’s in the food-as-medicine space — announced last week that it will offer co-branded MA plans with Alignment Healthcare that offer nutritious food programs for seniors starting in 2024.
Instacart also launched a partnership with Mount Sinai’s employer and union provider to give post-operative and post-partum patients grocery stipends.
Uber does not break out its health division publicly. However, the company says more than 3,000 organizations are working with Uber Health, and Uber Health reported 75% in gross bookings growth from 2022 to 2023.