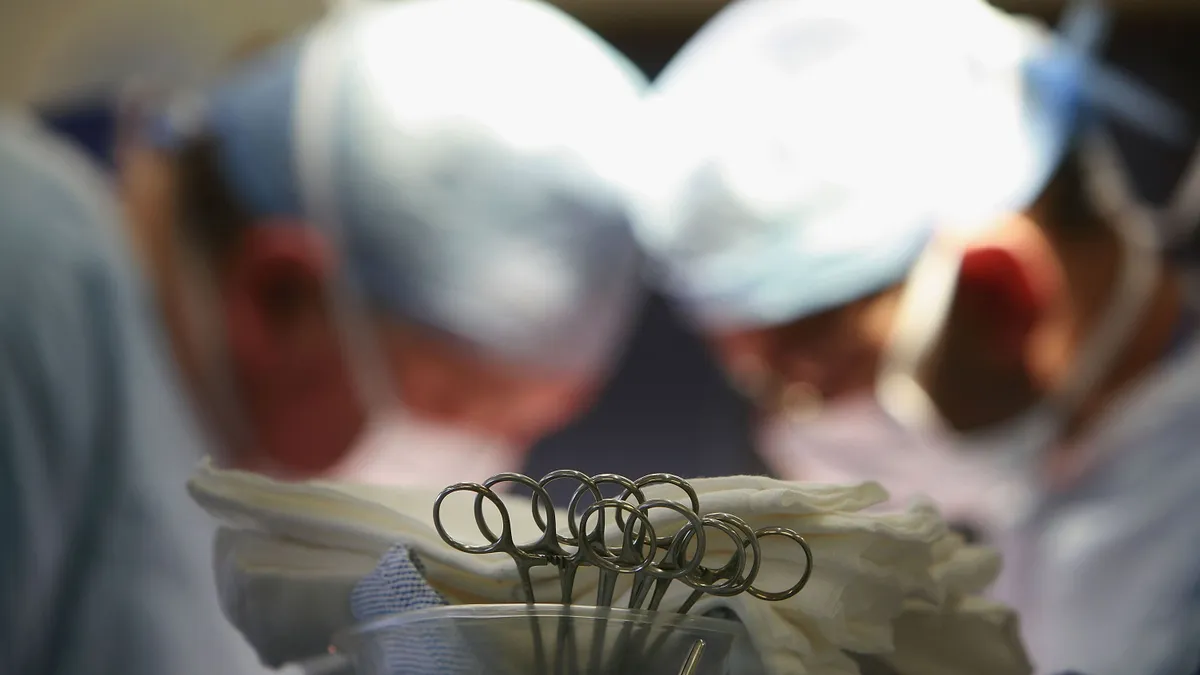
The coronavirus pandemic may necessitate temporary bumps in Medicare funding to providers, but an influential congressional advisory group recommended no massive hikes in payment for 2022, despite ongoing calls for additional aid from provider lobbies.
Regardless of having just gone through one of the most atypical years in Medicare payment ever, the Medicare Payment Advisory Commission is issuing "fairly conservative recommendations," largely due to a deficit in data on how COVID-19 affected the national health insurance program, Jim Mathews, executive director of MedPAC, told reporters Monday.
"We are doing our best efforts to prognosticate what might happen in 2022," based on available information, Mathews said.
To the extent that the effects of the pandemic are temporary and vary significantly depending on provider, they're best addressed through targeted yet temporary funding policies instead of permanent increases in all providers' payment rates that would cost the program more over time, MedPAC said in its annual report released Monday.
Congress has already implemented a significant amount of financial relief for cash-strapped providers in a flurry of COVID-19-related legislation last year and early this year. Legislators voted last year to up provider Medicare payments by 2% to insulate them from the worst of the pandemic's financial effects, though that relief expires at the end of this month.
Provider groups have also aired concerns that the passage of the $1.9 trillion American Rescue Plan, signed into law by President Joe Biden on Thursday, could trigger a decade-old budget neutrality provision. The measure, called pay-go, requires automatic payment cuts if any piece of legislation creates a net increase in the deficit.
The Congressional Budget Office estimates pay-go could require reductions in Medicare spending by 4% in 2022 if Congress doesn't intervene.
The American Hospital Association, American Medical Association and Federation of American Hospitals are among those pushing for an extension of higher Medicare payments as the pandemic slogs into 2021.
However, large health systems are generally reporting healthy profits despite fluctuating volumes last year. And indicators from 2019 suggest increasing payments from Medicare, a program relied on by tens of millions of Americans for coverage that's rapidly approaching insolvency, may not be the best solution for providers' purported fiscal woes, the MedPAC report suggests.
Researchers analyzed payment inadequacies in fee-for-service Medicare to determine how Congress should update Medicare's payment rates in 2022. MedPAC, which is required by law to submit recommendations annually, bases its suggestions on factors like beneficiaries' access and use of care, the quality of that care and other data like providers' costs.
MedPAC included some preliminary effects of the pandemic in its report, but researchers noted data from last year is still being collected and that they relied predominantly on 2019 data.
The goal of the recommendations is to lower Medicare spending while maintaining beneficiaries' access to care, MedPAC says. It's an important task: According to the CBO, the trust fund that finances Medicare's hospital benefit will run dry by 2024, two years earlier than previously expected due to the effects of COVID-19, without meaningful legislative action or spending cuts.
MedPAC recommends Medicare payments to acute care hospitals and long-term care hospitals should be increased by 2% for inpatient and outpatient services, which should result in a small net increase to hospitals' Medicare revenues in 2022.
The group recommends payment rates to physicians, ambulatory surgical centers, outpatient dialysis facilities, skilled nursing facilities and hospice services remain unchanged from current law. Asked about rising expenses for physicians during COVID-19, Mathew noted it's a valid concern but "at the moment all of our indicators are positive enough" to maintain the status quo.
MedPAC also recommended a 5% cut in payments to home healthcare agencies and inpatient rehabilitation facilities, and that the aggregate hospice cap, which governs how much payment a hospice can receive from Medicare in a given year, be wage-adjusted and lowered by 20%.
Besides the hospital update, the recommendations are in line with current payments or lower, so in aggregate would produce Medicare savings. If enacted, they would extend "the life of the Medicare trust fund for at least a few more minutes," Mathew said.
The suggested rates are likely to please some provider groups and incense others following a year of intense financial volatility. However, previous research suggests provider losses stemming from the pandemic haven't been as dire as initially feared.
MedPAC's report also analyzed the state of the Medicare Advantage program, which unlike fee-for-service Medicare is increasingly robust, researchers said. Enrollment, beneficiary access to MA plans and rebate levels that fund extra benefits all reached record highs in recent years, MedPAC found, noting a whopping 43% of all Medicare beneficiaries enrolled in the privately run Medicare plans last year.
However, Medicare shelled out $317 billion to MA plans in 2020, representing significantly higher per-beneficiary spending than in fee-for-service Medicare. Despite record-low plan bids for 2021, MedPAC estimates MA payments will be about 101% to 104% of fee-for-service spending this year.
As a result, some MA policies need "immediate improvement," MedPAC said, noting CMS could lower excess payments stemming from plans' coding practices resulting in excess payments and replace the MA quality bonus program with a different value incentive program that would more accurately reward quality of care.
The report also includes a policy option for Medicare's coverage of telehealth after COVID-19. There's broad bipartisan support for permanently lowering long-codified restrictions to telemedicine in the U.S. as utilization of digitally delivered care skyrocketed during the pandemic. However, current flexibilities will expire at the end of the public health emergency without legislative action, and the exact shape of any permanent reform is still being debated in the halls of Congress.
MedPAC suggests Congress expand coverage under Medicare for all beneficiaries beyond the PHE for a temporary period such as one or two years to give regulators more time to gather data about virtual care's efficacy and its impact on costs. However, Medicare should pay the lower physician fee schedule's facility rate for telehealth services, and providers also shouldn't be allowed to reduce or waive beneficiary cost-sharing as a safeguard against overutilization — a key worry among telehealth critics.
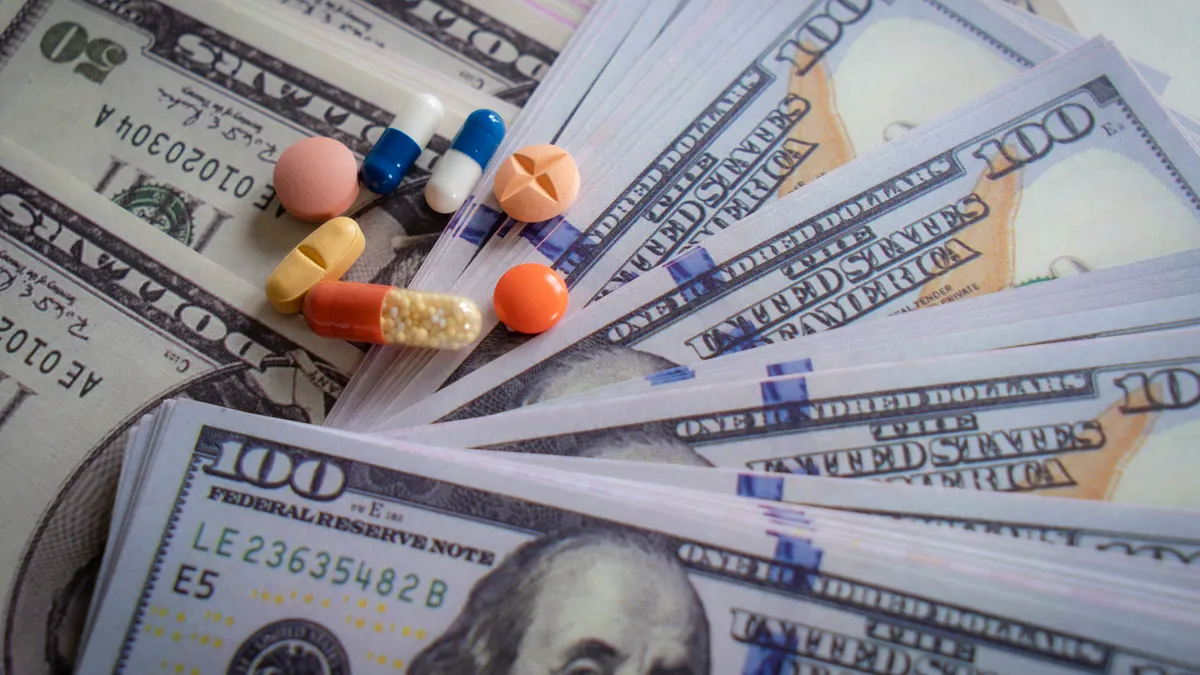
MedPAC also noted that, though Medicare's Part D prescription drug benefit continued to offer beneficiaries broad choice among plans and improve access to prescription drugs with few-to-no premium increases for many years, there's more the government could do to curb spending.
More of Medicare's payments to plans are in the form of cost-based reinsurance instead of fixed dollar payments, reducing plans' incentives to control spending. In addition, though overall Part D prices declined in 2019 due to increased use of generics, prices continued to rise in therapeutics dominated by brand-name drugs. Further inflation in drug prices among high-cost enrollees could continue to drive spending upward, MedPAC warned.
As a result, the commission recommends a facelift of Part D's benefit design to limit out-of-pocket costs, prioritize risk-based, capitated payments and nix features of the current program that distort market incentives.