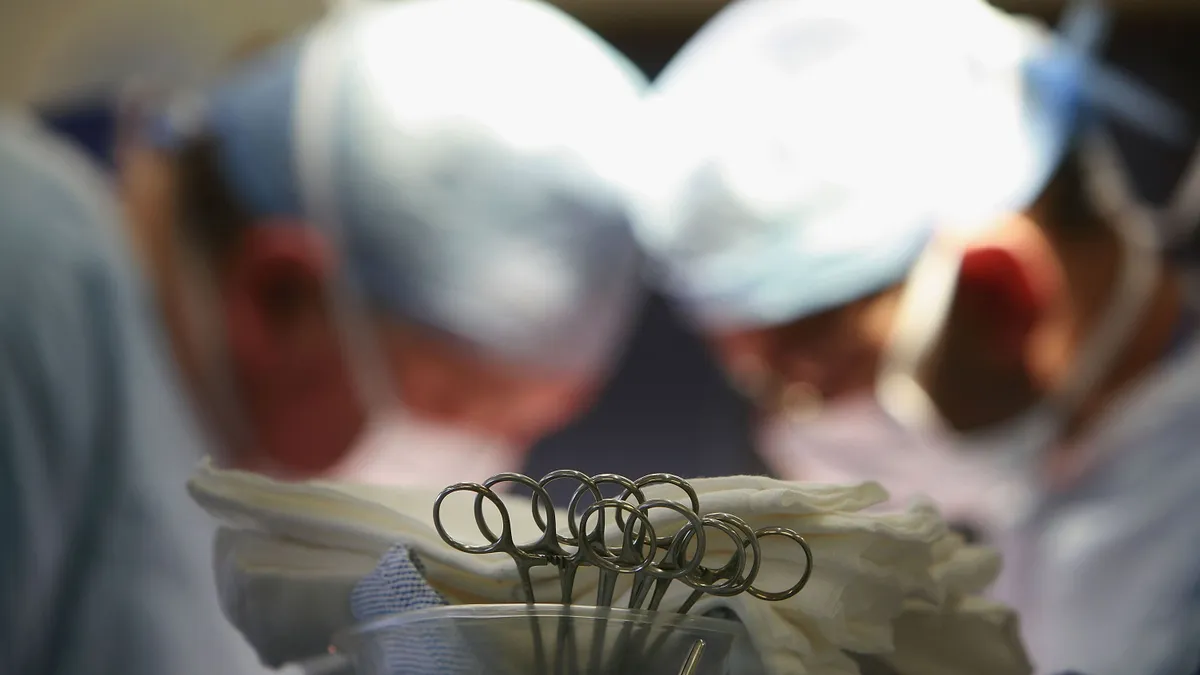
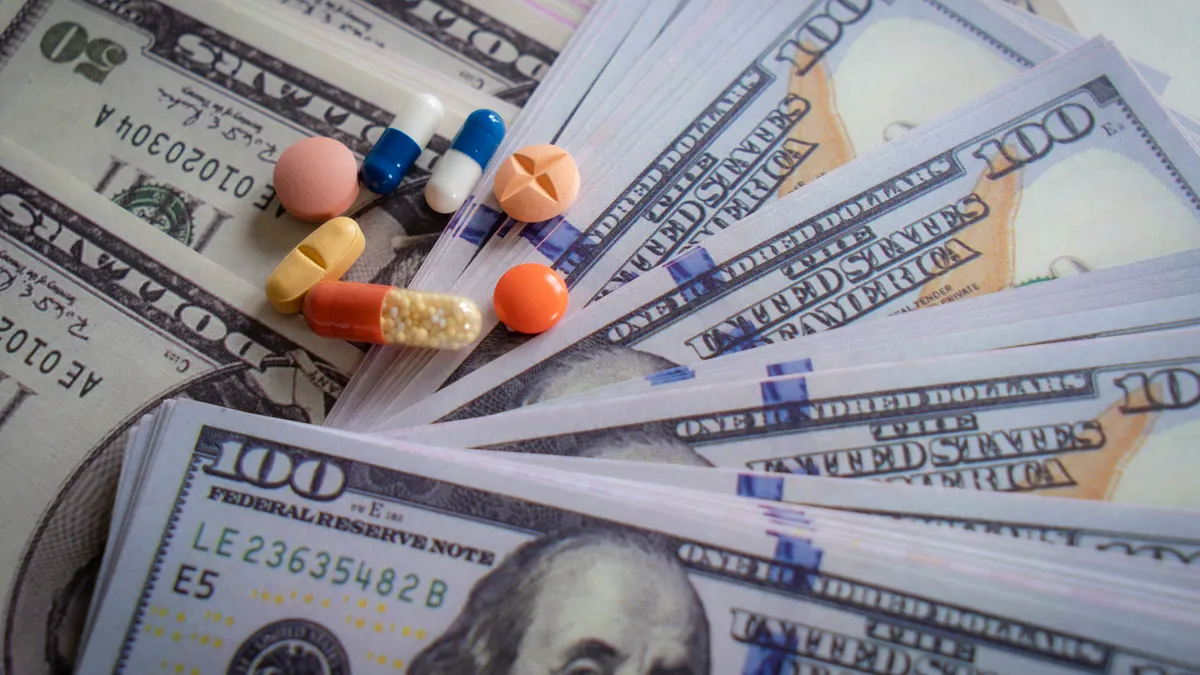
Maryland health insurance co-op Evergreen, which recently announced record financial results and its path to profitability for 2016, has been unique among the co-ops from the start. It stood secure as half the other co-ops had crumbled by late 2015, and its bullish outlook on 2016 is proving spot-on.
CEO Peter Beilenson attributes their success to three main factors.
The first is their diversified book of business, as opposed to a focus on individual enrollment, which prevented them from taking a devastating hit from the pent-up medical needs of new individual enrollees and the lack of expected risk corridor payments.
“We only have about 25%-30% of our book of business in the individual market. About 55%-60% is small group and 10%-15% is large group.” He adds they have fairly healthy and young populations in their small and large groups with a median age of 36.5, and a median age for individuals of 42.
Beilenson’s second factor is that from the beginning they priced their individual plans “appropriately,” not aggressively, which shielded them from excessive numbers of ill newcomers and meant they could cover those they had without reliance on the government’s unfulfilled risk corridor payments.
The third factor has been Evergreen’s heavy focus on wellness and prevention, Beilenson says. They are affiliated with the Evergreen Health Care system which provides primary care, health coaching, wellness centers, care coordination, and extra time with primary care physicians who are paid by salary rather than fee for service.
Beilenson credits this approach for their 10% reduction of ER visits and hospitalizations for their demographic.
What’s new in 2016
Evergreen is already surpassing their projected individual enrollment for 2016. “We’re about 30% ahead of our enrollment goals for the year already,” Beilenson says. He adds large group enrollment is right on target while small group is a little under where they want to be but progressing well.
“Our goal is to get to 53,000 or so by the end of this year and we’re currently at about 38,000 so 15,000 more is not a big lift.”
Beilenson says they are confident they will meet their enrollment goal and be profitable for the year, adding three of the last six months of 2015 were already profitable. “With a much bigger premium base and economies of scale as we get larger, conservatively speaking, we should make a modest profit.”
He is not concerned about their larger individual enrollment this year, because those coming in during this third year tend not to have the pent-up demand for medical care the first-wave of enrollees had. Many of them are the younger and healthier individuals who are choosing now to get insurance rather than pay the escalating penalty.
As for strategy, Evergreen will continue building on its wellness offerings, which have included education on diabetic nutrition and smoking cessation, and free or discounted access to other things of interest to members.
Beilenson says Evergreen is trying to meet the ACA’s intent of not only getting more people insured but doing things in an affordable way and bringing innovation to the market. To that end, they’re doing something no one else in Maryland is doing, he said, with their value-based insurance design (VBID).
For example, “If you are diabetic, we remove all the financial barriers to evidence-based care that studies show stop the progression of the disease and oftentimes cause it to reverse,” he says. “So for example, no co-pays, no out-of-pocket costs for a variety of tests, glucose strips, certain types of insulin, podiatry visits, eye doctor visits, endocrine visits, primary care visits, all the things that would prevent people with diabetes from getting into complicated diabetes.” That approach is keeping people out of hospitals, Beilenson says, and Evergreen will be adding an additional condition each year to that design.
“The sole remaining obstacle-–not just to the co-ops but to all small, new insurers is risk adjustment,” Beilenson says. Like many critics, he argues the current formula is heavily skewed toward the pre-existing larger insurers, in part due to grandfathering and the issue of up-coding to get higher risk adjustment scores, resulting in small insurers paying the big ones in a “ridiculous game of revolving dollars.”
With its influx of younger, healthier members, Evergreen could be hit hard for this year. “That is a potential,” he says, adding they’ll be ok because of their strong financials, but that some co-ops are expecting between 30 and 60% of their premium revenue to go out the door to their big competitors in their states. He argues if anything, insurers should be rebating that money to their members. He’s working to press CMS to institute a three-year cap of no more than 2% of premium as a payable for risk adjustment for any carrier in the country until 2018, at which time the grandfathering will be over and many hope the formula will be changed.
Beilenson says it’s unfortunate the ACA currently dis-incentivizes VBID because those not providing strong services see their patients progress to higher level codes and receive better reimbursements.
“So by doing the right thing, we are actually being penalized,” he notes.