Payer: Page 2
-
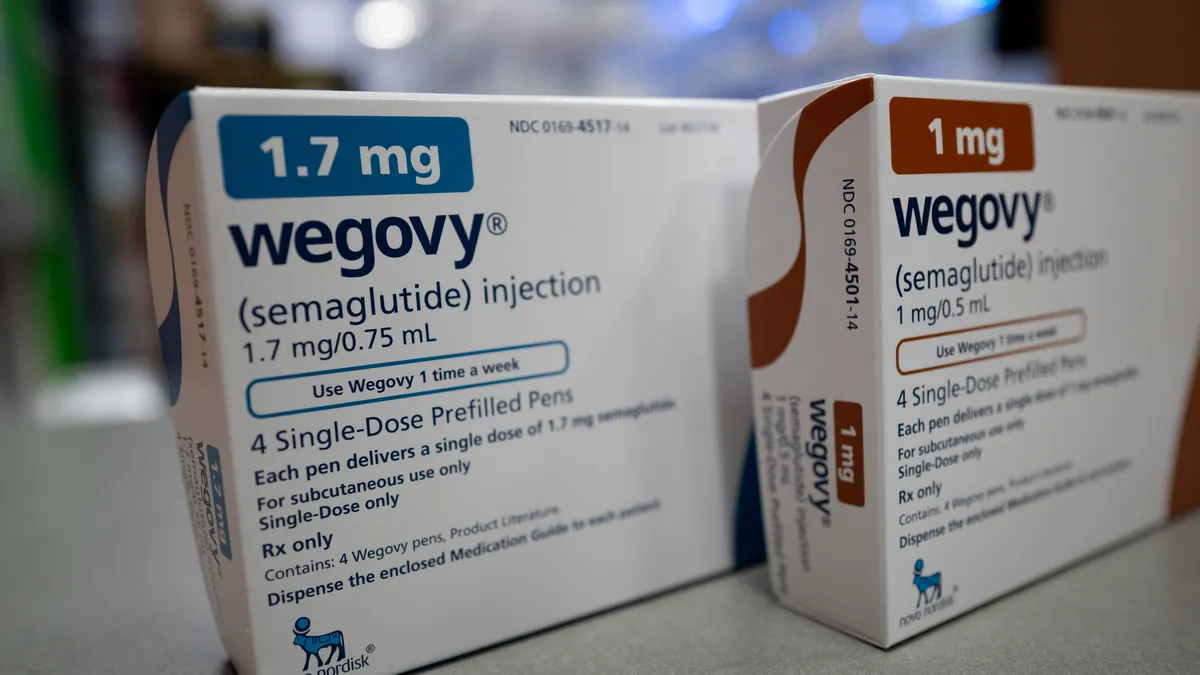
CFOs feel healthcare pain rising as GLP-1s stretch budgets: Mercer
Average healthcare costs for U.S. employers are expected to rise 6.7% this year, hitting a 15-year high.
By Alexei Alexis • April 22, 2026 -
Prices rose after No Surprises arbitration for some care: analysis
The data compiled by the Brookings Center on Health Policy shows that average arbitration prices for some services like imaging were seven times higher than Medicare prices.
By Sydney Halleman • April 22, 2026 -
 Explore the Trendline➔
Explore the Trendline➔
 Yujin Kim/Healthcare Dive
Yujin Kim/Healthcare Dive Trendline
TrendlinePayer/provider relationships
As M&A intensifies and companies embrace more holistic and value-based care models, partnerships have become more closely intertwined.
By Healthcare Dive staff -
Elevance perks up in 2026 though Medicare Advantage payout could ding profits
The Indianapolis-based insurer raised its 2026 earnings guidance after posting a better first quarter than Wall Street expected. Still, Elevance lodged a $935 million expense to cover what it might owe the CMS over faulty data reporting.
By Rebecca Pifer Parduhn • Updated April 22, 2026 -
UnitedHealth hikes profit outlook after better-than-expected first quarter
Premium hikes, plan redesigns and other efforts from the Minnesota-based company to wrangle medical spending bore fruit in the first quarter. UnitedHealth’s stock jumped accordingly.
By Rebecca Pifer Parduhn • April 21, 2026 -
Blue Shield of California taps chief pharmacy officer
Hayley Park will oversee BSCA’s prescription drug programs. The insurer has worked to overhaul its pharmacy management model in a bid to lower drug costs.
By Emily Olsen • April 21, 2026 -
Judge dismisses Aetna’s No Surprises fraud suit against Radiology Partners
The insurer accused the radiology group of gaming the No Surprises Act to reap higher reimbursement. A judge tossed the case last week, saying Aetna needed to raise its complaints during the dispute resolution process.
By Emily Olsen • April 20, 2026 -
Sponsored by Counsel Health
3 questions every payer should ask about medical AI
As medical AI scales, how are payers ensuring safe and compliant care?
April 20, 2026 -
Stakeholders urge Labor Department to finalize PBM transparency rule
Employers, lawmakers and more said regulators should hustle to get disclosure mandates for the controversial drug middlemen across the finish line, while PBMs slammed the rule as illegal, unnecessary and anticompetitive.
By Rebecca Pifer Parduhn • April 17, 2026 -
More employers considering medical, pharmacy vendor switch amid rising healthcare costs, survey finds
Healthcare affordability continues to keep employers up at night. More businesses are shopping for new healthcare vendors as a result, according to the Purchaser Business Group on Health.
By Rebecca Pifer Parduhn • April 16, 2026 -
ACA exchanges will continue to shrink as fewer enrollees pay premiums, analysis suggests
About 14% of ACA enrollees didn’t pay premiums in January, a higher rate than usual and one that suggests ACA enrollment will continue to decline, according to Wakely.
By Rebecca Pifer Parduhn • April 16, 2026 -
More insurance claims denials are being overturned upon appeal, study finds
Study authors, who reviewed data from New York, said rising rates of overturned claims suggest that insurers’ claims review processes might not be working as intended, and policymakers should consider getting involved.
By Rebecca Pifer Parduhn • April 15, 2026 -
CMS accepts more than 150 providers, digital health firms for ACCESS model
Participants will receive set reimbursement for managing Medicare beneficiaries’ chronic conditions, like diabetes, chronic kidney disease and hypertension.
By Emily Olsen • April 14, 2026 -
Surprise Billing
California judge tosses Elevance’s surprise billing suit in win for providers
It’s a major victory for controversial billing intermediary HaloMD, which cheered the court’s decision. Elevance said it plans to appeal.
By Rebecca Pifer Parduhn • April 14, 2026 -
Medicare proposes 2.4% pay bump for inpatient hospitals in 2027, floats mandatory model
Regulators are proposing to send $1.4 billion more to acute care hospitals and debut the first nationwide, mandatory payment model to lower the cost of joint replacements. Hospitals pushed back.
By Sydney Halleman • April 13, 2026 -
CMS proposes new deadlines for prior authorizations for drugs
Drugs were left out of a 2024 rule streamlining prior authorizations by making decisions electronic and requiring payers to turn them around more quickly. The Trump administration is looking to address that gap.
By Rebecca Pifer Parduhn • April 13, 2026 -
Sponsored by PointClickCare
From afterthought to advantage: How health plans are rethinking post-acute care
From reactive to proactive, how plans are transforming post-acute care management.
April 13, 2026 -
ICHRAs, a growth opportunity for insurers, face uphill battle
Employers are turning to Individual Coverage Health Reimbursement Arrangements to cut costs, but rising premiums and instability on the individual market pose challenges.
By Michael Brady • April 8, 2026 -
Jefferson Health sues Aetna over Medicare Advantage ‘downcoding’ policy
The health system claims the policy, which reduces reimbursement for some inpatient hospital stays, violates federal law and its reimbursement contract with Aetna. The insurer disagreed with Jefferson’s allegations.
By Sydney Halleman • April 8, 2026 -
CMS finalizes higher Medicare Advantage rates for 2027 in gift to insurers
Regulators locked in a 2.48% rate hike for next year, much higher than the 0.09% that was proposed. Analysts said the Trump administration was likely spooked about coverage disruptions for seniors before the midterm elections.
By Rebecca Pifer Parduhn • April 7, 2026 -
Insurers committed to cutting prior authorizations have eliminated 11% so far
Last summer, major payers committed to pare back onerous prior authorization policies, to the skepticism of providers. Now, AHIP and the Blue Cross Blue Shield Association are providing an update on insurers’ progress.
By Rebecca Pifer Parduhn • April 7, 2026 -
Sponsored by CVS Caremark
Standing up to rising prescription drug costs increases access to breakthrough medications
For millions of Americans, accessing the medications they need at prices they can afford has gotten increasingly difficult.
By Dr. Michelle Gourdine, Senior Vice President, CVS Health; Chief Medical Officer, CVS Caremark • April 7, 2026 -
Centene creates two new executive leadership roles
It’s the latest in a flurry of executive appointments from health insurers looking to strengthen their leadership teams amid regulatory headwinds and elevated medical costs.
By Rebecca Pifer Parduhn • April 6, 2026 -
CMS finalizes Medicare Advantage star ratings overhaul, sending billions of dollars more to insurers
Regulators cut almost a dozen metrics that factor into the quality ratings and reverted back to an older and more generous bonus system. MA plans will get more than $18 billion in additional payments over the next decade as a result.
By Rebecca Pifer Parduhn • April 3, 2026 -
Bipartisan lawmakers urge CMS to crack down on Medicare Advantage overpayments
Senators praised a recent CMS proposal aimed at reducing payments in MA, but urged the agency to work with Congress and go further.
By Emily Olsen • April 1, 2026 -
Elevance sidesteps Medicare Advantage sanctions for now
The insurer had until the end of March to correct faulty data submissions or be hit with severe sanctions from the CMS. But regulators agreed to give Elevance more time to comply.
By Rebecca Pifer Parduhn • April 1, 2026