The COVID-19 pandemic has had a profound effect on the healthcare industry, and nearly two years after it began, organizations are still grappling with the challenges they faced when it started. While the popularity of telehealth medicine soared in 2020, 2022 has seen this remote healthcare option become a mainstay in provider practice. Although it is convenient for patients and providers, substantial compliance risks are still involved in telehealth medicine.
In addition, recent enforcement actions by the US Department of Justice (DOJ) have pointed to specific risks organizations may face during a merger or acquisition. These settlements demonstrate the importance of practicing due diligence and resolving liabilities that originated before a merger or acquisition. A looming recession may also require healthcare organizations to adopt a “back-to-basics” mentality regarding compliance monitoring. But achieving compliance during a recession is not without its unique challenges.
Keep reading to learn about healthcare trends we’ve noted from the past year and how you can stay compliant in 2023.
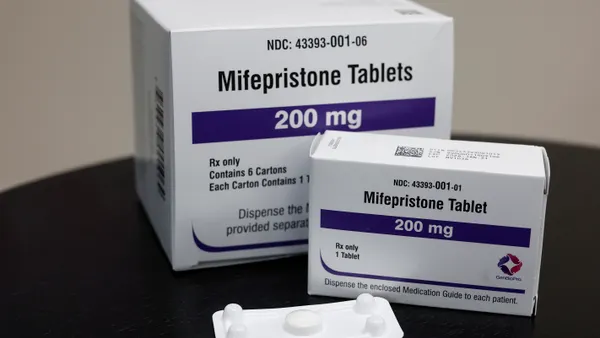
Trend #1 – Scrutiny in Telehealth Medicine
The COVID-19 pandemic highlighted our country’s widespread appetite for virtual care and expanded telehealth services. The option to access healthcare services from the comfort of one’s home has become something many patients look for when seeking a new provider. In fact, according to McKinsey, around $250 billion in outpatient spending could potentially shift to virtual settings in the coming years. However, telehealth medicine isn’t exempt from today’s compliance risks.
With more people receiving telehealth care, ensuring your organization and providers remain compliant with healthcare laws and regulations is more important than ever. Telemedicine fraud can take many forms, including up-coding (submitting incorrect billing codes to insurance companies to receive inflated reimbursements), misrepresenting a virtual service, billing for services not rendered, and kickbacks.
As with brick-and-mortar practices, it’s still critical to ensure your providers’ licenses and credentials are in good standing. However, license and exclusion monitoring can be a tedious process. Still, patient safety remains a top priority as more people opt for virtual care. By making license and exclusion monitoring a part of daily compliance and HR workflow, organizations can help ensure their providers are properly licensed and eligible to provide care to their patients.
Donna Thiel, Chief Compliance Officer at ProviderTrust, describes the importance of adjusting processes to maintain compliance. “Telehealth has expanded in a way that, so far, consumers and regulators all seem to think is good. They’re wanting to continue it, so how are you going to change your processes to meet those requirements? We [ProviderTrust] look at all providers every single day across all states and hundreds of licensing boards to help our clients ensure that their telehealth providers are compliant and can provide care throughout the United States. Reducing the risk and creating efficiencies makes ProviderTrust an invaluable partner.”
Learn more about combatting telehealth fraud in our blog post, Top Compliance & Security Risks in Telehealth.
Trend #2 – Due Diligence in Mergers & Acquisitions
In recent years, certain enforcement actions and settlements by the US Department of Justice (DOJ) have demonstrated that company buyers continually resolve liabilities that originated before their ownership. However, whether or not the buyers were aware of the conduct prior to closing is not always clear.
In 2017, Quest Diagnostics settled with the DOJ for $6 million to resolve a lawsuit alleging improper kickbacks provided by Berkley HeartLab, which Quest acquired in 2011. Similarly, in 2017 Genesis Healthcare agreed to pay $53.6 million to settle False Claims Act allegations regarding medically unnecessary therapy and hospice services and sub-standard nursing care provided by entities acquired by Genesis. All allegations related to pre-acquisition activities.
Given the breadth of enforcement in the healthcare space and the astronomical settlement amounts, buyers must understand that they may be held responsible for past noncompliance, including liability for past fraud and abuse violations and billing improprieties. It is therefore vital for companies to practice due diligence when merging or acquiring a new entity, as liability may also transfer over with this change of hands.
Trend #3 – Compliance During a Recession
An August 2022 survey of CEOs by McKinsey found that “81 percent of leaders expect a recession.” Rising interest rates and inflation also seem to indicate that our economy may be headed in a downward direction. Recessions affect healthcare fraud and compliance in many ways. During economic downturns, there is often a rise in criminal activity. Increased fraud volume is typical, as are criminal activities of cybersecurity and ransomware attacks. In addition, businesses often cut out non-revenue-generating activities during a recession, and compliance is often a target for financial curtailing.
Knowing an economic slump is coming and preparing for it ahead of time can help your organization combat these recession challenges. Regular risk assessments are a great place to start. Are your providers’ licenses in good standing? Do you have cybersecurity protocols in place to prevent hacking or ransomware attacks? A well-funded compliance effort should also still be prioritized despite pressures to minimize expenses and personnel. Educating and training employees to understand fraud risks can help foster a culture of compliance as well.
Above all, and despite the financial difficulties a recession presents, your organization’s duty to provide upstanding patient care should not be compromised. As you navigate a recession and focus on remaining financially viable, remember the importance of communicating values and how to conduct business compliantly.
About ProviderTrust
ProviderTrust simplifies and automates the license monitoring process for healthcare's top HR and compliance teams. ProviderTrust provides daily exact-match results from the primary source. This allows healthcare organizations to focus on their patients, with in-house and contracted staff, while ensuring credentials are always in good standing. Accessible healthcare does not have to compromise the standard of care.
Ensure your providers are properly licensed for telehealth and avoid the risk of fraud in mergers and acquisitions as well as an impending recession by learning more about ProviderTrust's license monitoring solution.