Apple's latest iPhone can store 256 billion bytes of information. The Hubble Space Telescope collects 10 trillion bytes every year.
But healthcare companies have both technologies beat. Express Scripts, one of the nations biggest pharmacy benefit managers, keeps roughly 22 petabytes of healthcare data. That's about the same storage as 16 billion floppy disks or 86,000 of the new iPhones.
The company is learning a great deal about its 80 million members from this staggering amount of data — from where they live to their medical history. And with the help of complex algorithms, so are its computers.
Artificial intelligence, a technology that has drawn pharma's interest with the promise of supercharging computer-aided drug discovery, has in recent years also caught the attention of the prescriber side of the market. So far it's unclear exactly what effect AI will have on prescribing, though experts generally agree it will be quite awhile, if at all, before the technology starts making decisions in place of a doctor or pharmacist.
Rather, payers and big tech companies are exploring how AI can help healthcare providers make more informed decisions for patients.
"If you think about prescribing, there's been a bit of technology involved in assisting prescribers in making the right decision for a very long time," Tina Moen, deputy chief health officer at IBM Watson Health, told BioPharma Dive. "AI is the next step, the next evolution of that."
The evolution won't happen overnight, however, as the technology continues to mature and prescribers, who largely operate autonomously, weigh the pros and cons of giving machines a seat at the table.
A win-win for payers?
Healthcare tech company Philips is among those diving deeper into AI.
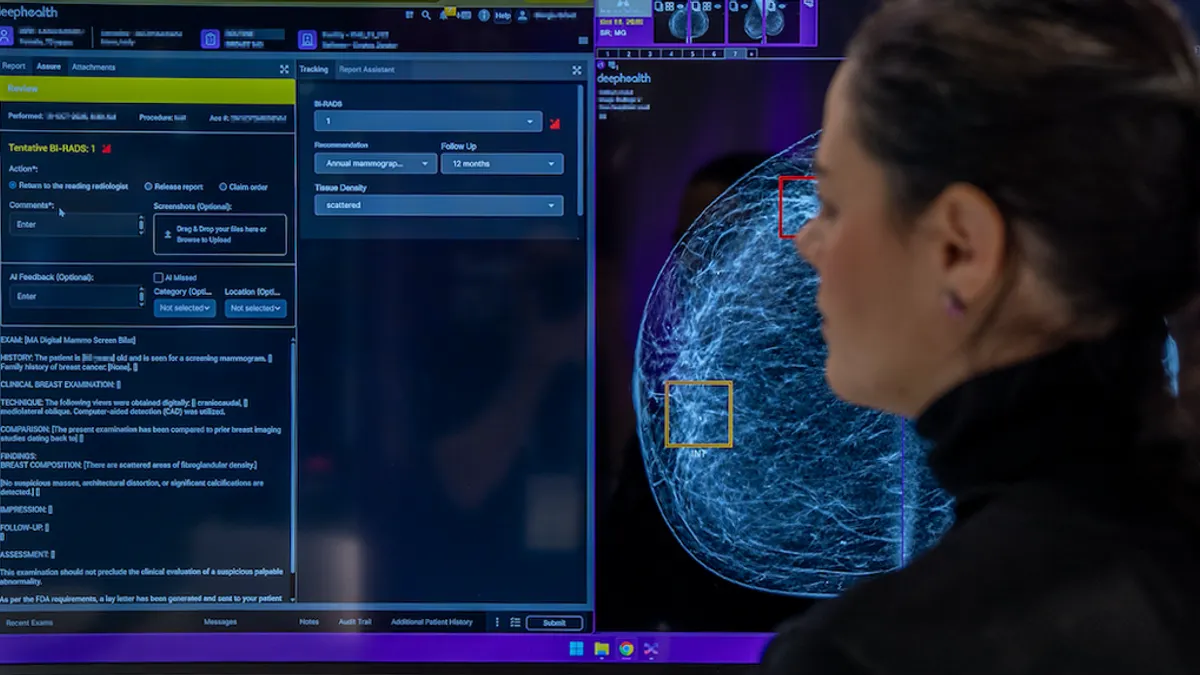
The technology was at the center of its 2017 collaborations with PathAI and Nuance Communications, aimed at improving diagnostic decision-making and outfitting radiologists with more sophisticated tools and reporting capabilities. Just last month, Philips said it would be deploying the Dana Farber Cancer Institute's Clinical Pathways, a knowledge-sharing system for oncologists, into its AI-backed IntelliSpace Oncology Platform, which collects and organizes data to improve cancer treatment.
The deals illustrate the many ways in which AI could be useful for doctors, but payers also see potential. Anthem, for instance, has been open about its interest in leveraging big data analytics and machine learning to better understand its customers. For many insurers and PBMs, the tech could be a win-win — making the prescribing process potentially safer and faster while also building formularies that protect bottom lines.
"Probably the group that would be most interested would be payers, and I would think it would be almost like a quality control check," Louis Culot, general manager of oncology informatics and genomics at Philips, told BioPharma Dive.
Culot noted that payers already use rules engines, a type of computational model that suggests an action based on what are essentially a series of if-then prompts, to approve or deny reimbursement requests. AI offers a more advanced version of this, pulling from massive data sets of clinical trial information, real world evidence and more to determine whether there's a less risky treatment option available.
Patient benefit still an open question
In one example, Express Scripts is using AI and big data platforms to navigate filling opioid prescriptions amid a national overdose epidemic.
"[W]e do that by taking the millions and millions of members that we have data on and identifying all of those people that have an opioid dependency diagnosis, and then training the machine on: What are the common features that resulted in that diagnosis in that group of individuals?" said Tom Henry, chief data officer at Express Scripts, in an interview with BioPharma Dive.
Express Scripts can then draw data-driven conclusions about how people from a certain geography or demographic group are likely to respond to a given therapy.
"Those people that are at high risk, we want to intervene if they're prescribed an opiate very quickly to say, 'Hey, this is a pretty dangerous substance. Let us help you manage that,' as opposed to just having it sent to a person and have them go unchecked," Henry added.
Elsewhere, the company is targeting patient and operational costs. Aided by its recent $3.6 billion acquisition of medical benefit management provider eviCore healthcare, Express Scripts is using machine learning and natural language processing to alleviate some of the burden associated with prior authorizations (PAs), an extra layer of approval required by some insurers to fill certain prescriptions.
"Improving the process by using data to inform the decision reduces cost because we're not taxing as many of our clinicians, but also improves the experience of the member at least in the eviCore space of having these PAs approved in an automated, much quicker way," Henry said.
Doctors warm to new tools
While payers speed toward AI, practitioners seem to be taking a more tempered approach.
That's not to say they aren't enticed by new technologies. A 2016 physician survey from the American Medical Association found that among 1,300 responders, 85% said patient care would benefit from digital health solutions.
But IBM's Moen notes that many healthcare professionals have come to view AI with a "cautious optimism," similar to how they treat a new class of medicine.
"There's apprehension on the adoption because of that sort of sanctity of healthcare and how personal it really is at the end of the day, particularly for the patient," she told BioPharma Dive.
For tech firms, the task then becomes not only developing and integrating healthcare AI tools, but showing how they'll enhance, rather than upend, the doctor-patient relationship.
"Obviously, the computers can't meet the patient and have the sort of dialogue [physicians can]," Culot said. To that point, IBM, Philips and others have presented their AI platforms as a kind of prescriber assistant, putting information that's not easily accessible in front of doctors so they have more time to meet with the patient and a fuller view of the treatment options.
"They know the first-line therapy, they learned that in school," Moen said. "It's when that first line therapy is inappropriate for some reason — patient's allergic, there's a drug interaction — that's where technology and AI really shine."
What's left to code?
But AI's shining moment hasn't yet arrived, at least not in drug development and prescribing.
Like most new technologies, there have been setbacks. The most notable came in early 2017, as a partnership between IBM Watson and MD Anderson Cancer Center that sought to use AI in cancer treatment decisions didn't live up to expectations despite years of work and more than $60 million worth of investments.
IBM continues to asses Watson's health applications, having to date processed nearly 60,000 patient cases and brought the technology to 230 hospitals and health organizations. The company also announced on July 19 it would be extending a partnership with the Department of Veterans Affairs so that the agency's oncologists can use the Watson Genomics platform through at least June 2019.
Still, there's more work to be done.
"One of my biggest learnings, and something that we ... continue to take very seriously is the idea of: How do we share with the market? How do we educate the market on what's behind the AI?" Moen said. "The last thing we want at Watson Health and broader IBM is for our AI solutions to seem like a black box of any sort."
Making the AI platforms more accurate is another priority, but that relies on robust data and advanced computations. One project in that vein can be found at Stanford University, where researchers have developed an AI platform that models expected side effects for patients taking multiple drugs.
Decagon, as the project's called, pulls from datasets to construct a multimodal map of interactions between proteins, between drugs and between proteins and drugs. Though Decagon was unveiled only recently, the creators told BioPharma Dive that several companies have acknowledged its potential uses, like in shaping better hypotheses at earlier stages of drug development.
Yet where it could be most useful is in prescribing newly approved drugs, according to Jure Leskovec, an associate professor of computer science at Stanford and part of the Decagon team.
"All you have to tell us is what proteins will this drug target, and we can immediately make predictions about what side effects this would cause if this drug would be taken in combination with some other drug," he said.